Progesterone is important for women’s health. Yet for decades, it has been ignored or wrongly blamed for side effects it doesn’t cause. How did that happen?
A missed opportunity
Progesterone was discovered shortly after estrogen, missing the chance to be included in the simplified narrative of “testosterone for men and estrogen for women.” To complicate things further, progesterone couldn’t initially be made into an oral medication, so it was sidelined in favor of synthetic progestins.
In contrast, early formulations of testosterone (testosterone propionate, 1940s) and estrogen (estradiol valerate, 1960s) were body-identical—that is, structurally identical to hormones made by the body. As a result, they were the focus of clinical research. But body-identical progesterone (oral micronized progesterone) didn’t become available until the 1990s.
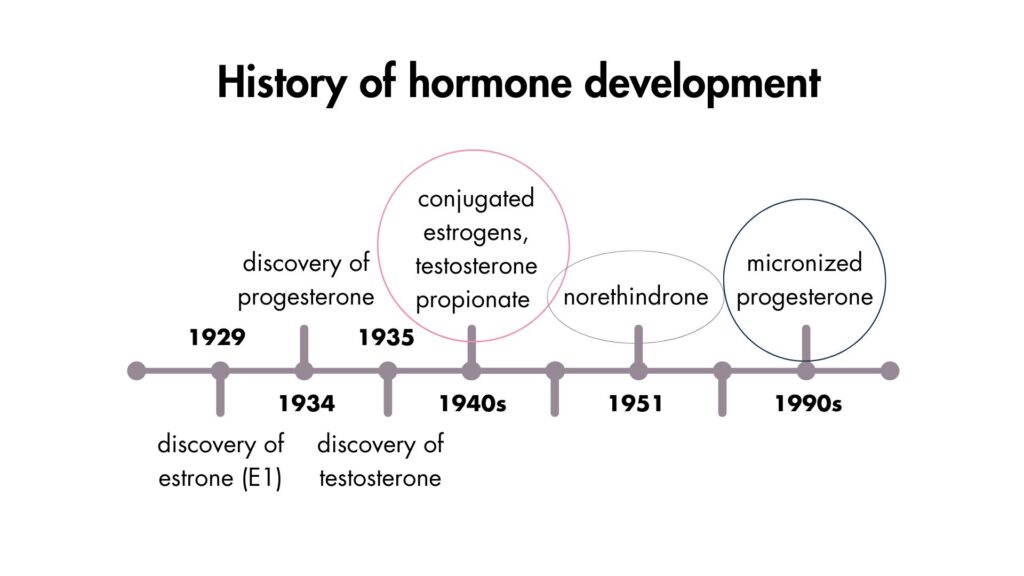
That delay meant that most early research was done on synthetic progestins, not progesterone.
💡Did you know? Estrogen is a generic term that includes both natural estradiol and synthetic compounds like ethinylestradiol. Progesterone, on the other hand, refers specifically to the natural hormone. It does not include progestins.
Progesterone ≠ progestins
Progestins are not the same as progesterone. In fact, they can have different (and sometimes opposite) effects. For example:
- All progestins slightly increase the risk of breast cancer
- Progesterone may reduce the risk of breast cancer
Despite this, many of the risks and side effects of progestins have long been misattributed to progesterone.
Fortunately, this is starting to change. Experts now recognize that body-identical progesterone is safer than progestins.
Progesterone and estradiol work as a team
It’s time to re-center real progesterone in the conversation, because (just like estrogen), it’s important for long-term brain, bone, and heart health. It also works in synergy with estradiol on many tissues. For example, estradiol promotes ovulation and increases progesterone receptor activity. In turn, progesterone balances estradiol’s effects:
| Estradiol | Progesterone | |
|---|---|---|
| Uterus | Thickens the lining | Thins the lining |
| Brain | Stimulates | Calms |
| Breasts | Promotes cell growth | Slows cell growth |
Progesterone also plays a key role in regulating the hypothalamus and promoting healthy ovulation.
💡Did you know? A healthy luteal-phase progesterone level is around 80 nmol/L, which is 100 times higher than the average peak estradiol level of 800 pmol/L (0.8 nmol/L).
Together, estradiol and progesterone protect the brain, bones, and cardiovascular system. In the words of Professor Jerilynn Prior:
“Ovulatory cycles across a woman’s long reproductive life span are needed to prevent osteoporosis and fracture, heart attacks, and breast and endometrial cancers during women’s older years.”
Each ovulatory cycle is like a deposit into the bank account of long-term health.

Do you make progesterone?
The only way to make progesterone is to ovulate.
- An ovulatory cycle is a menstrual cycle in which ovulation occurs and progesterone is produced.
- A non-ovulatory (anovulatory) cycle lacks ovulation and progesterone. These are more common than many people realize.
💡Tip: Knowing if and when you ovulate is called body literacy.
For more, see:
- My books Period Repair Manual, Hormone Repair Manual, and Metabolism Repair for Women
- A safer type of hormone therapy
- The right way to test progesterone
- Roadmap to progesterone
- Guide to using progesterone for women’s health
