
In women, too much testosterone can promote insulin resistance and visceral fat.
That’s why androgen excess is the primary driver of weight gain with polycystic ovary syndrome (PCOS), some types of birth control, and perimenopause.
PCOS and weight gain
With PCOS, high ovarian androgens cause insulin resistance or high insulin. High insulin can then stimulate ovarian cells to make more testosterone, creating a vicious cycle and all the resulting symptoms of weight gain, acne, facial hair, irregular periods, and an increased long-term risk of type 2 diabetes.
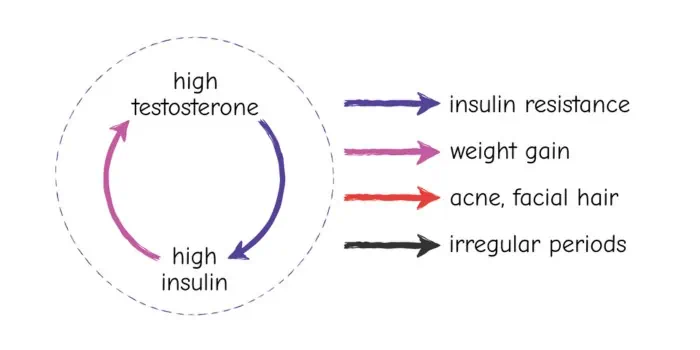
Breaking the cycle
Treatment with natural progesterone can disrupt this cycle by lowering androgens, improving insulin sensitivity, and promoting ovulation. Notably, Professor Jerilynn Prior’s lab has just completed a clinical trial of cyclic progesterone therapy for PCOS.
💡 Tip: Progestins in hormonal birth control are not the same as body-identical progesterone. Many progestins are actually androgenic or testosterone-like.
Birth control and androgens
Some progestins in hormonal birth control are androgenic, which can cause insulin resistance and weight gain. The most androgenic progestins include:
- Levonorgestrel
- Norethindrone
- Etonogestrel
These are commonly found in pills, Nuvaring, Mirena IUD, and the Nexplanon implant. Combination with synthetic estrogen (as with combination pills and Nuvaring) tends to offset the androgenic effect to some extent.
Anti-androgenic progestins
On the other hand, anti-androgenic progestins, such as drospirenone, norgestimate, dienogest, and cyproterone, can improve insulin sensitivity and promote weight loss. However, stopping an anti-androgenic progestin can lead to rebound weight gain.
Perimenopause, menopause, and testosterone
During perimenopause, levels of progesterone and then estrogen decline, while androgens slightly (temporarily) increase. This creates a situation of “relative androgen excess,” where testosterone is relatively high compared to estrogen and progesterone.
Fat redistribution
Androgen excess encourages fat to shift from subcutaneous areas (such as the hips and thighs) to visceral areas (inside the abdomen), resulting in a thicker waist and heavier upper body.
Hormone therapy
Treatment with body-identical estradiol and progesterone (rather than a progestin), can improve insulin sensitivity and counteract testosterone’s effects by increasing sex hormone-binding globulin (SHBG) and other mechanisms.
💡 Tip: Be careful with testosterone medication, as too much can cause or worsen insulin resistance.
For more treatment ideas, see my book Metabolism Repair for Women.
